Verify Insurance for Rehab in Massachusetts: What Coverage Really Means
In 2000, Massachusetts did something most states hadn’t.
While Congress was still debating the edges of a narrow federal parity law, one that equalized annual and lifetime dollar limits but left everything else untouched, Massachusetts passed its own law, An Act Relative to Mental Health Benefits, going much further than existing federal legislation by mandating coverage for biologically based mental health conditions.
Most states waited. Massachusetts moved. Then in 2008, the law was broadened again to mandate coverage for medically necessary treatment for substance use disorders, eating disorders, post-traumatic stress, and autism.
This is not a footnote. It is the foundation on which every conversation about rehab coverage in this state now stands. Massachusetts did not inherit these protections. Advocates fought for them, bill by bill, amendment by amendment, over the course of a decade. That history matters to you right now because the rights it produced are real, enforceable, and almost certainly broader than you have been led to believe.
The problem is that nobody hands you a pamphlet at the moment you need it most.
The Gap Between Coverage And Care Is Where Most People Get Lost
You know you have insurance. You may even know, in some general sense, that mental health and substance use treatment are covered. What you are less likely to know is that coverage and approval are not the same thing and that the distance between them is measured not in months or paperwork but in the precise words a clinician uses to describe your need for treatment.
Before most insurers authorize rehab, they require a prior authorization: a formal determination that your treatment is medically necessary.
This determination is not made by anyone who has met you. It is made by a reviewer at the insurance company, working from criteria you were never shown, applying standards you were never given the opportunity to address.
The process is not designed to deny you care.
Yet, it is also not designed around your readiness, your timeline, or the particular Wednesday afternoon when something finally shifted and you decided you were ready to go.
Many consumers still find it more difficult to access mental health or substance use treatment than other types of health care because of insurance limits.
Not because the laws failed, but because knowing the law exists and knowing how to use it are entirely different things.

The Questions That Really Matter And Why Most People Never Ask Them
Most people approach insurance verification with one question: Is rehab covered? That question is not wrong. It is just the first sentence of a much longer conversation that most people don’t know they need to have.
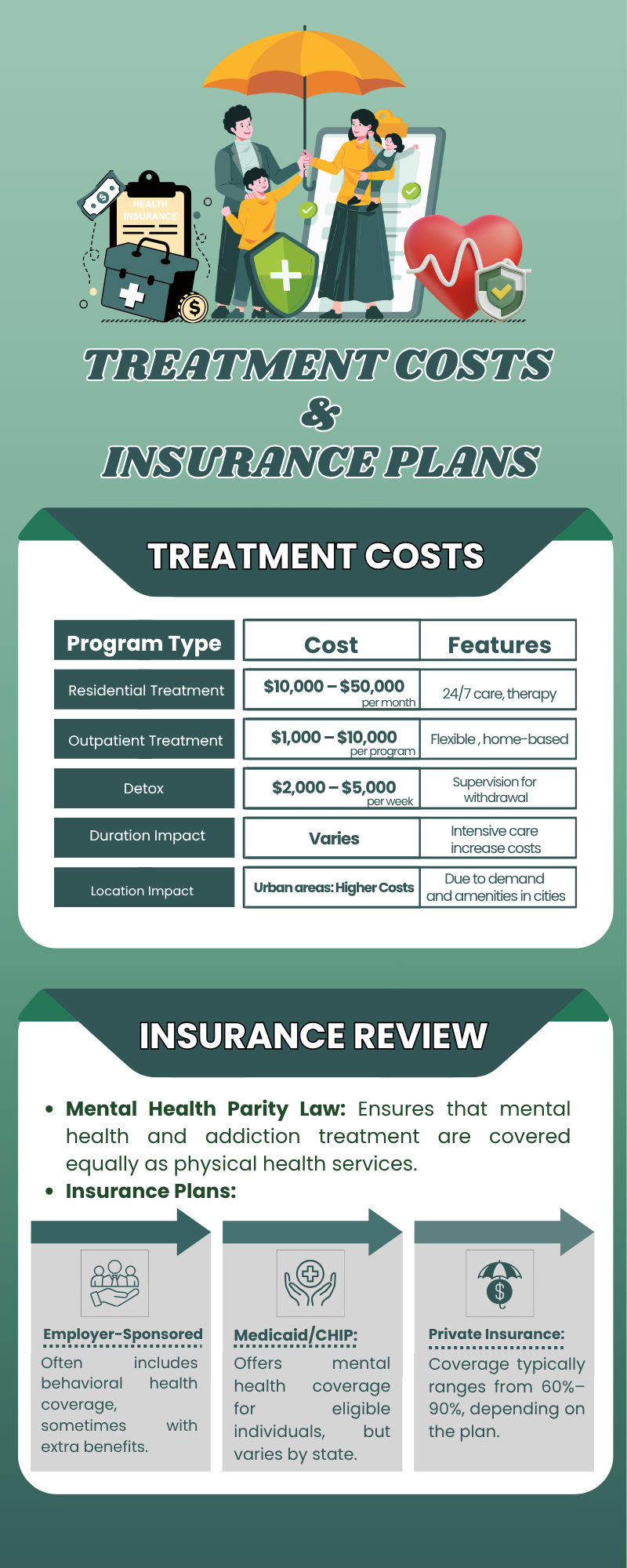
The questions that follow are the ones that determine what your experience will actually look like:
- Is this facility in-network, or will you be billed at out-of-network rates for every session?
- What level of care does your plan cover, including detox, residential, partial hospitalization, and/or intensive outpatient?
- What is your deductible, and critically, how much of it remains for this calendar year?
- Is prior authorization required, and if so, what clinical documentation does your insurer need before they will issue it?
- What is your out-of-pocket maximum, and what happens to your cost share once you reach it?
These are not bureaucratic boxes to check. They are the difference between a bill that arrives three months into recovery at the exact moment you are most fragile and least equipped to fight it and one that doesn’t.
The Law That’s On Your Side And How To Use It
The Federal Parity Law, the Affordable Care Act, and the Massachusetts Parity Law together provide strong protections for Massachusetts residents with mental health or substance use conditions. Health insurance policies must offer benefits for mental health care in the same service categories covered for medical and surgical benefits. This means if a plan covers inpatient care for physical illness, it must cover inpatient care for substance use treatment as well.
There is a practical application to this that most people never reach. If your insurer covers unlimited outpatient visits for a physical condition, it cannot legally apply a stricter cap to addiction treatment. If it covers inpatient cardiac rehabilitation without a session limit, it cannot impose one on residential rehab. The Massachusetts Mental Health and Substance Use Parity Coalition has worked to secure regulations requiring the Division of Insurance and MassHealth to issue and enforce parity protections. Hence, there is a state agency whose job is specifically to investigate complaints when insurers don’t follow these rules.
What Happens When You’re Denied And Why Denial Is Not The End
Denials happen. They follow a recognizable script: a determination that your condition does not meet medical necessity criteria for the level of care requested, or a requirement that you demonstrate failure at a lower level of care before a higher one will be authorized. These denials feel final in the moment. They are frequently not.
Appeals succeed at rates most people would find surprising, often between 40% and 80%, if most people ever filed them. What stops them is not the process itself. Rather, it is the weight of fighting a system while simultaneously trying to get better. Advocacy organizations are well positioned to recognize common parity issues, assess possible violations, and bring them to the appropriate state office, but only if someone helps you find them. This is where your treatment provider matters as much as your insurance card.
A program that knows how to document medical necessity, how to respond to a denial in the specific language your insurer responds to, and how to file an appeal that addresses the actual criteria in question. That program changes your odds. Significantly.
What Real Insurance Verification Looks Like
There is a meaningful difference between a program that accepts your insurance and a program that actively works it on your behalf. The first means your carrier is on their list. The second means someone who does this every day, checks your specific plan, confirms your deductible, identifies whether prior authorization is required, and files it with the right documentation the first time, so the approval comes before you arrive, not after.
At Clover Behavioral Health, insurance verification begins before your first session. Not as a formality. As a complete accounting of what your plan covers, what it will cost you, and what comes next. The major commercial carriers like Aetna, Blue Cross Blue Shield, Cigna, United Healthcare, Humana, and others are verified in real time, not estimated.
Massachusetts spent decades fighting for your right to this coverage. The least you deserve is someone who knows how to claim it.
Call us or reach out through our website. Bring your insurance card and your questions. We’ll tell you exactly what your plan covers, what it will cost, and what happens next.
The coverage exists. Let us show you how to reach it!