Does Insurance Cover Mental Health Treatment in MA?
There is a specific kind of quiet that lives between knowing you need help and actually reaching for it. Not silence exactly. More like the sound of a tab opened and closed. A number written down and never dialed. A thought that arrives at 2am and is almost gone by morning. Just present enough to make the next day harder.
Part of what sustains that quiet is a question that feels too large and too uncertain to ask out loud: will any of this even be covered? It is a question about whether the path forward is truly open to you.
In Massachusetts, it is. The coverage exists, it is legally protected, and it is more specific and more enforceable than most people ever discover. What follows is not a general reassurance. It is a direct answer to what your insurance covers, what the law guarantees, and what to do with that information today.
The Short Answer And Why It Matters
Yes. In Massachusetts, insurance is required to cover mental health treatment. Not as a courtesy extended by your carrier. Not as a benefit subject to quiet elimination at renewal. As a legal obligation, enforced by state law, federal law, and a regulatory body whose job is specifically to investigate complaints when insurers fall short.
The Federal Parity Law, the Affordable Care Act, and the Massachusetts Parity Law together provide strong protections for Massachusetts residents with mental health or substance use conditions. Health insurance policies must offer benefits for mental health care in the same service categories covered for medical and surgical benefits. This suggests that if a plan covers inpatient care for physical illness, it must cover inpatient care for mental health treatment as well. The same applies to outpatient, emergency, and prescription medications.
Moreover, financial requirements like deductibles and copayments generally cannot be any more restrictive for mental health treatment than for medical or surgical care. If your plan charges you a $30 copay to see your primary care physician, it cannot legally charge you $60 to see a therapist.
Most people who have been quietly absorbing that difference for years never knew they had grounds to push back.
What Masshealth Covers And Who It Reaches
Commercial insurance is not the only pathway. Massachusetts residents enrolled in MassHealth have access to coverage for medically necessary mental health and substance use disorder services, with all respondent carriers covering services for diagnoses as defined in the most current clinical standards.
MassHealth eligibility is based on income, household size, and Massachusetts residency. Not employment status, not prior coverage history, not the nature of the condition being treated. Coverage includes outpatient therapy, intensive outpatient programs, partial hospitalization, crisis services, and psychiatric care. For those who qualify, the barrier is not coverage. It is knowing the coverage exists and finding a provider who accepts it, which is a navigable problem, not an impossible one.
The Massachusetts Health Connector serves residents who don’t qualify for MassHealth but purchase coverage independently. All Connector plans are required to include mental health and substance use treatment as essential health benefits, with the same parity protections that apply to employer-sponsored plans.
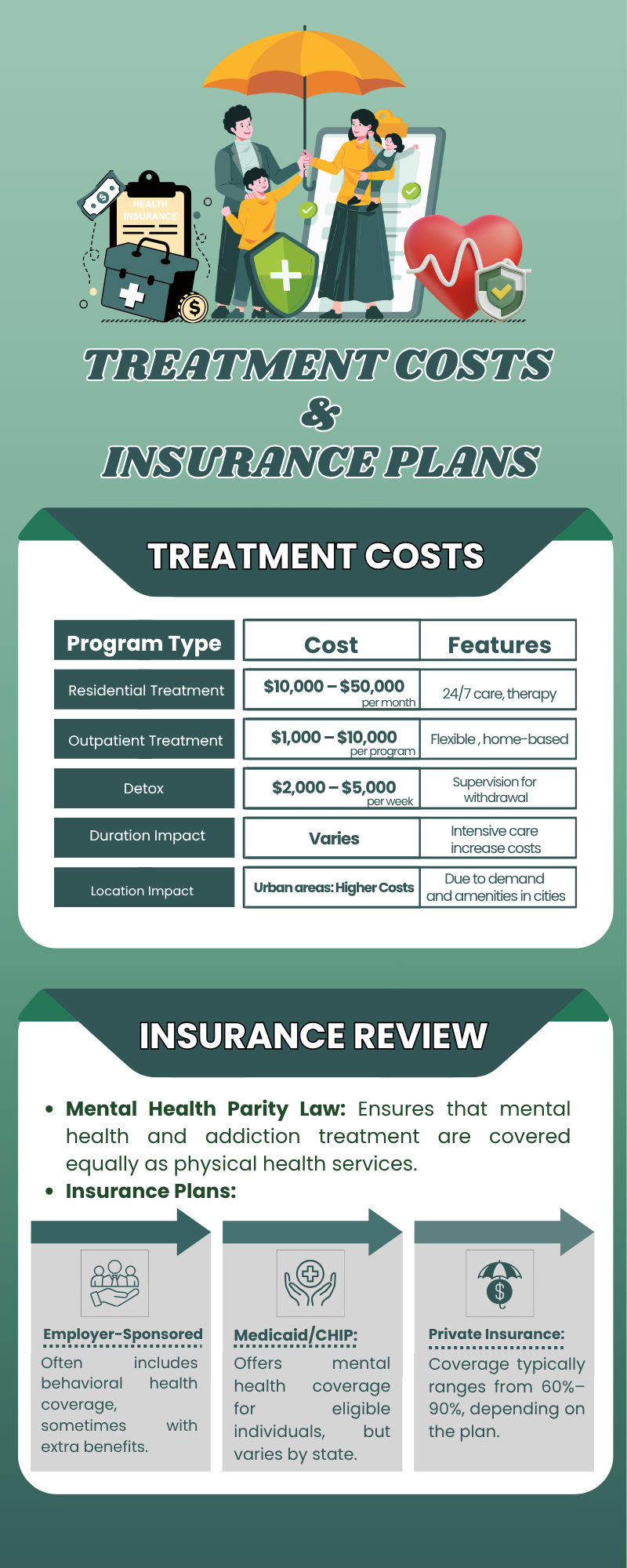

The One Thing Coverage Doesn’t Eliminate
None of this removes prior authorization from the picture. Most commercial plans still require a formal determination that your treatment is medically necessary before IOP, PHP, or inpatient care will be approved. That determination is made by a reviewer who has not met you, working from criteria you were not given the opportunity to address in advance.
Even in the more than fifteen years since the federal parity law’s enactment, people still encounter barriers to accessing mental health and substance use disorder care compared to medical and surgical care under their health plan. The law closed the gap in what is owed. It did not eliminate the machinery that sometimes stands between what is owed and what is delivered.
The Massachusetts Division of Insurance requires that health insurers provide all enrollees with information on their rights under parity laws and how to file a complaint. Hence, when an insurer falls short, there is a formal process for holding them to account. Most people never use it. Knowing it exists changes the conversation before it ever reaches that point.
Five Questions That Cut Through The Confusion Before Your First Session
The law guarantees coverage. It does not guarantee you will automatically understand what that coverage means for your specific plan, your specific provider, and your specific situation. These five questions, asked and answered before treatment begins, replace uncertainty with a clear picture:
- Is this provider in-network under my plan, or will I be billed at out-of-network rates?
- Does my plan require a referral from a primary care physician before I can access mental health services?
- Is prior authorization required for the level of care I need, and if so, what clinical documentation triggers approval?
- What is my copay or coinsurance per session, and does it differ by level of care?
- What is my out-of-pocket maximum, and how much of it remains for this calendar year?
These are not complicated questions. They are simply ones that nobody asks you to ask until the bill arrives.
What Does Clover Do? Real Answers, Not Estimates
There is a difference between a program that lists your insurance carrier as accepted and one that reads your specific plan, verifies your specific benefits, and tells you exactly what your mental health treatment will cost before anything begins. The first offers possibility. The second offers clarity.
At Clover Behavioral Health, benefits verification happens before your first session and covers every variable that matters. Deductible status, copay by level of care, prior authorization requirements, and in-network confirmation. Major commercial carriers – including Aetna, Blue Cross Blue Shield, Cigna, United Healthcare, and Humana – are verified directly and in real time. If your situation involves MassHealth or the Health Connector, that conversation happens with the same transparency.
Ready To Take the First Step?
Call us or connect through our website. Bring your insurance card and whatever questions have been sitting unanswered. We will tell you exactly what is covered, exactly what it will cost, and exactly what happens next.
The coverage is real. So is the clarity. Let us show you both!