Does MassGeneral Brigham (AllWays) Insurance Cover Rehab? What You Need to Know
Health insurance doesn’t always feel straightforward, especially when you’re trying to access rehabilitation or behavioral health care.
There’s rarely a clear moment when you suddenly know what’s covered, what’s not, and what comes next.
Instead, there are questions. Phone calls. Policy language that feels clinical when the situation is deeply personal.
That’s where understanding your insurance coverage matters.
For many people in Massachusetts and surrounding areas, MassGeneral Brigham Health Plan, formerly known as AllWays Health Partners, is a major local carrier that plays an important role in access to rehab and behavioral health services.
Knowing what this coverage typically includes, and how to use it, can make the difference between delaying care and getting support when it’s needed.
Why Rehab Coverage Matters
Rehabilitation services, including treatment for substance use disorders and mental health conditions, are not optional add-ons to health care. They are essential.
National data shows that people with insurance coverage are significantly more likely to seek and remain engaged in treatment compared to those without coverage.
In Massachusetts, insurers are required to follow both federal and state laws, including the Mental Health Parity and Addiction Equity Act, which mandates that mental health and substance use disorder benefits be comparable to physical health benefits.
MassGeneral Brigham Health Plan operates within this legal framework, making behavioral health and rehab services a standard part of many plans rather than an exception.
What Is MassGeneral Brigham (AllWays) Insurance?
MassGeneral Brigham Health Plan is the insurance division of Mass General Brigham, one of the largest and most respected healthcare systems in the United States.
Previously known as AllWays Health Partners, the organization transitioned to the MassGeneral Brigham name to better reflect its connection to the broader hospital and provider network. While the name changed, the focus remained the same: offering coordinated, accessible care across a wide range of medical and behavioral health needs.
The plan includes multiple coverage options, including employer-sponsored plans, individual marketplace plans, and Medicaid managed care options through the Massachusetts Health Connector.
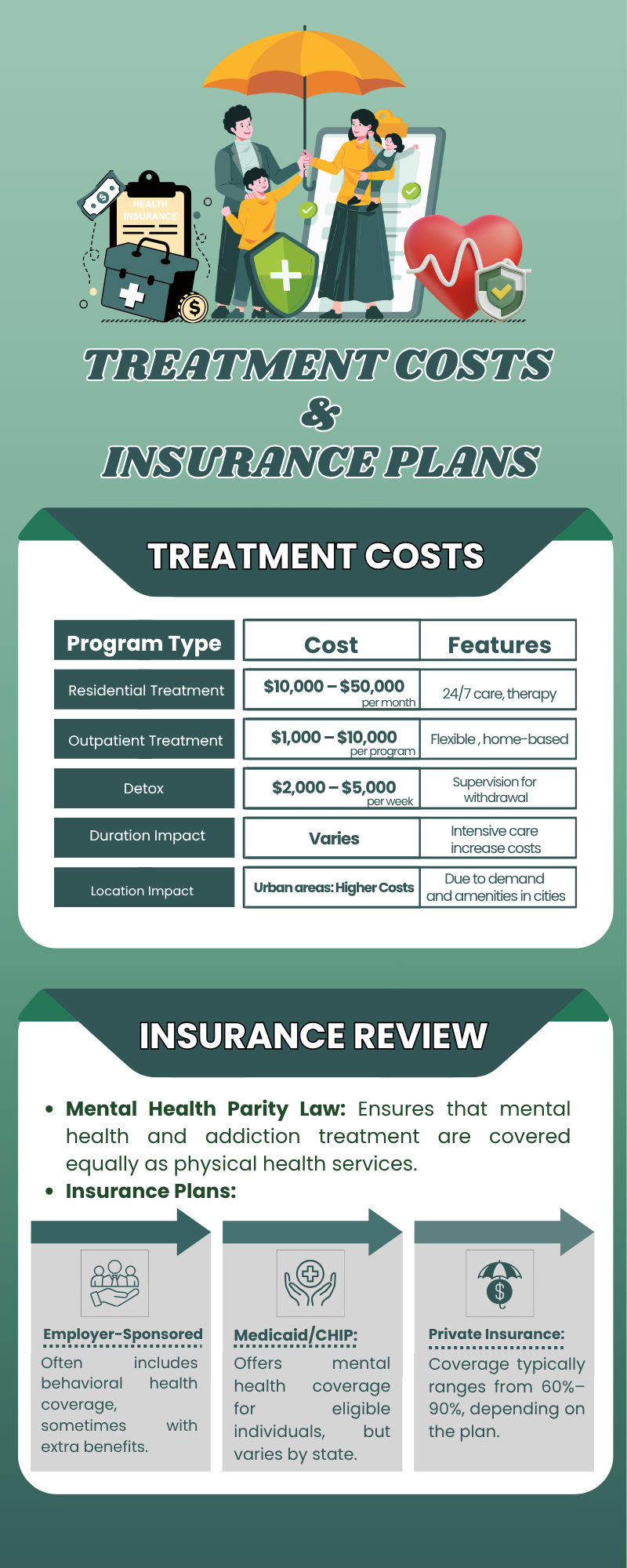
Behavioral Health and Rehab Coverage: What’s Typically Included
Coverage details always depend on the specific plan, but MassGeneral Brigham (AllWays) insurance generally includes behavioral health and rehabilitation services as part of its core benefits.
For many members, this means access to care across different levels of treatment based on clinical need.
These services often include outpatient therapy and counseling, detoxification programs, residential or inpatient rehab, partial hospitalization, intensive outpatient programs, medication-assisted treatment, and care coordination services.
Whether and how these services are covered depends on factors such as medical necessity, provider network participation, and whether prior authorization is required.
Understanding Medical Necessity
Medical necessity is one of the most important concepts in rehab coverage.
It refers to whether a specific service or level of care is clinically appropriate based on diagnosis, severity, and individual needs.
Insurance providers use medical necessity guidelines to determine what type of treatment is covered and for how long.
This doesn’t mean care is unavailable. It means that proper assessments, documentation, and provider recommendations play a central role in accessing coverage.
Understanding this term can help reduce confusion, delays, and unexpected denials when seeking treatment.
Rehab Services You May Be Able to Access
Many MassGeneral Brigham plans include coverage for medically supervised detox, which is often the first step in treating substance use disorders. Detox services focus on managing withdrawal symptoms safely while preparing individuals for ongoing treatment.
For those who need more intensive support, inpatient or residential rehabilitation may be covered when it is considered medically necessary and provided by an in-network facility. These programs offer 24/7 structure and clinical care in a supportive environment.
Outpatient and intensive outpatient programs are also commonly covered. These options allow individuals to receive structured treatment while continuing to live at home, making them a practical choice for many people depending on clinical recommendations.
Coverage may also extend to co-occurring or dual-diagnosis treatment, which addresses mental health conditions and substance use disorders at the same time.
Integrated treatment is widely recognized as a more effective approach for long-term recovery and is supported under parity laws.
How to Check Your Rehab Benefits Without Guesswork
Understanding your benefits early can prevent unnecessary stress later.
Starting with your insurance card is helpful, as it includes your plan type and the member services phone number.
When contacting customer service, asking directly about behavioral health and substance use disorder treatment coverage can provide clearer answers than general benefit questions.
Requesting a benefits summary can also be useful. This document explains covered services, out-of-pocket costs, and whether prior authorization is required.
Confirming that a rehab provider is in-network can significantly reduce expenses.
For individuals who find insurance navigation overwhelming, support organizations like Clover Behavioral Health can help review benefits, explain coverage details, and guide people toward treatment options that align with their plan.

A Local Carrier
As a major Massachusetts-based insurer connected to a large hospital system, MassGeneral Brigham Health Plan plays a meaningful role in access to behavioral health and rehab services across the region.
Its size and integrated network allow for coordinated care, but understanding plan details remains essential to using benefits effectively.
Many members are able to access a wide range of providers, programs, and levels of care when they know how referrals, authorizations, and in-network rules work.
Clear knowledge of coverage can reduce delays in treatment and help people make informed decisions during stressful situations.
Insurance works best when people know how to use it, especially when timely access to care can directly impact recovery and long-term outcomes.
Final Thoughts
Rehab coverage isn’t just a line item buried in an insurance policy.
It represents real access to care at moments when support matters most, often during periods of crisis, transition, or recovery.
When people understand what their insurance covers – behavioral health benefits, medical necessity requirements, and provider network rules – it becomes easier to move forward without unnecessary delays or confusion.
MassGeneral Brigham (AllWays) insurance can help make rehabilitation and behavioral health treatment more manageable when benefits are used effectively.
With clear information and the right guidance, navigating coverage becomes less overwhelming and more about taking a confident, informed step toward care and stability.