A Simple Guide to Tufts Health Plan Mental Health & Substance Use Coverage
Behavioral health care doesn’t come with a pause button. It doesn’t wait until paperwork is complete, the calendar is clear, or something suddenly feels easier. It shows up in real life, stress that won’t shift, anxiety that stays sharp, or habits and thoughts that just don’t feel manageable anymore.
When those moments arrive, having insurance that supports behavioral health care can make a real difference.
For many people in Massachusetts and surrounding states, Tufts Health Plan is one of the carriers that stands between uncertainty and meaningful access to care.
Tufts Health Plan provides coverage for a range of mental health services, from outpatient therapy to intensive programs for complex needs.
But understanding what’s covered and how your benefits work is the first step toward getting help when it matters most.
Knowing your plan details early helps avoid unnecessary delays, reduces confusion, and allows members to access the right care promptly.
Why Behavioral Health Coverage Matters
Behavioral health needs are common. National data shows that in 2022, 23% of U.S. adults received mental health care in the past year.
A notable increase from previous years, and adults with insurance are far more likely to receive care than those without coverage.
In fact, insured adults received mental health treatment at more than double the rate of uninsured adults – 25% vs. 11%.
Other research using the National Survey on Drug Use and Health also shows that expanded insurance coverage through policies like the Affordable Care Act is associated with significant reductions in being uninsured among adults with mental and substance use disorders, and modest increases in mental health treatment use after coverage expands.
Insurance coverage doesn’t automatically solve every access challenge; many insured people still report difficulties finding in-network providers but it does create a foundation for care that wouldn’t exist otherwise.
What Is Tufts Health Plan?
Tufts Health Plan is a well-established health insurance provider serving individuals, families, and employers, with a strong presence in Massachusetts and neighboring states.
The plan offers a variety of coverage options designed to meet different needs, including employer-sponsored plans, individual marketplace plans, and, in some cases, public program products.
Across many of these options, behavioral health benefits, covering both mental health care and substance use services, are integrated into comprehensive health coverage rather than treated as separate or secondary add-ons.
This integration is important because behavioral health is an essential part of overall health.
Mental and physical well-being are closely connected, and insurance that supports both together helps individuals access care more effectively, leading to better overall outcomes and improved long-term wellness.
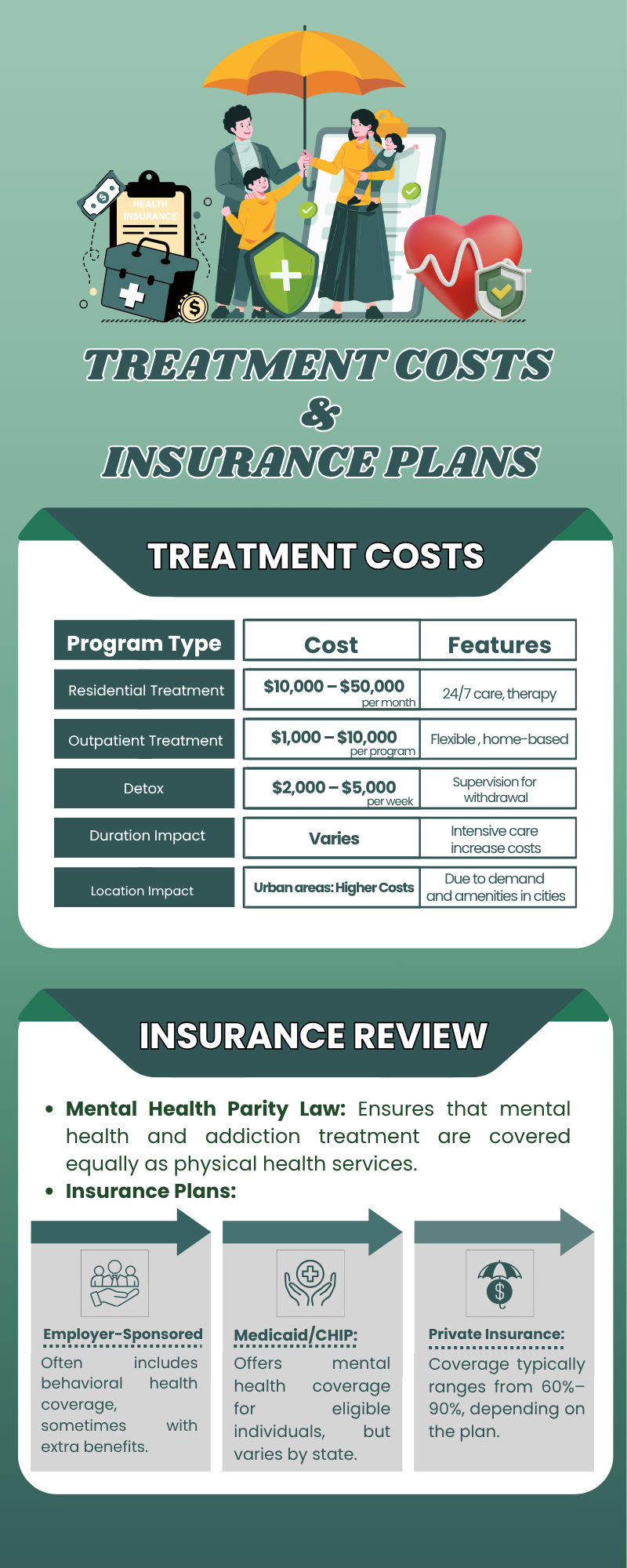
What Behavioral Health Benefits Look Like Under Tufts Health Plan
Exact benefit design depends on your specific plan, but most Tufts Health Plan members have access to a range of behavioral health services.
Many people can use their coverage for outpatient therapy and counseling for conditions like anxiety, depression, trauma, relationship stress, and more.
Psychiatric evaluation and medication management are generally included for those who need them.
For individuals facing more intensive challenges, coverage often extends to higher levels of care, including medically supervised detox, intensive outpatient programming, partial hospitalization, and residential treatment when clinically appropriate and medically necessary.
Behavioral health benefits may also include support for substance use disorder treatment and care coordination to help members stay engaged and connected to the right services at the right time.
Understanding Medical Necessity and Networks
One of the biggest pieces that determines access isn’t just what could be covered, it’s what’s considered “medically necessary.”
In practice, that means treatment must be appropriate based on clinical need, diagnosis, and level of severity.
Providers typically assess these needs and submit documentation to support authorization. Knowing which services require prior approval and which don’t can save time and stress.
Another reality is that network participation matters. Even when insurance covers services, finding providers who accept your plan can be challenging.
A recent survey found that many insured adults report difficulty finding in-network mental health professionals.
When you’re seeking help, confirming that a therapist, psychiatrist, or treatment program is in-network can reduce out-of-pocket cost and help care start sooner.

How to Check Your Behavioral Health Benefits
Getting clarity on your coverage doesn’t have to feel confusing. Start with a call to the number on your Tufts Health Plan member card. Ask specifically about behavioral health benefits, including outpatient services, substance use treatment, and requirements for prior authorization.
Requesting a benefits summary can help you understand covered services, copayments or coinsurance, and any limitations.
You can also confirm which clinicians and programs are considered in-network, something that really matters for cost and access.
If insurance language feels overwhelming, organizations like Clover Behavioral Health can help walk you through the details and connect you to providers who align with your plan.
A Plan With Benefits That Matter
Tufts Health Plan provides behavioral health coverage that can offer meaningful support for individuals navigating mental health concerns or substance use challenges.
Its coverage includes a wide range of services, from outpatient therapy and counseling to substance use treatment and intensive programs.
However, the real benefit emerges when members understand how to use their plan effectively and take full advantage of available care options.
Knowing exactly what services are covered, which requirements apply, and which providers are in-network transforms a policy from paperwork into a practical tool for care.
Insurance works best when people can navigate it confidently, access support during critical moments, and feel empowered to prioritize their mental and emotional well-being.
Final Thoughts
Behavioral health benefits aren’t just a box to check on a form; they represent access to care when vulnerability appears. They open a pathway from the first uncomfortable moment toward meaningful support that helps people navigate change and recovery safely.
Tufts Health Plan’s behavioral health coverage can make this journey more accessible when members understand the benefits, requirements, and provider networks.
Knowing how medical necessity works and where to seek in-network care reduces delays, confusion, and unnecessary financial stress later.
With clear information, thoughtful guidance, and trusted support resources, navigating coverage becomes less confusing and more confidence-building for people.